- Our Research
- Research Areas
- Addictions
- Aging & Geriatrics
- Behavior Change
- Biostatistics
- Cancer
- Cardiovascular Health
- Child & Adolescent Health
- Chronic Illness Management
- Health Informatics
- Health Services & Economics
- Healthy Communities
- Medication Use & Patient Safety
- Mental Health
- Obesity
- Preventive Medicine
- Social Determinants of Health
- Vaccines & Infectious Diseases | COVID-19
- Our Scientists
- Collaborate with Us
- Our Publications
- Research Funding Sources
- Research Areas
- News and Events
- Get Involved
- About Us
- Live Healthy
All Articles on Breast Cancer
- Few benefits seen for ultrasonograms for women with dense breasts
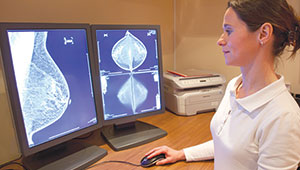
Dense breasts are a risk factor for breast cancer, and the more dense breasts are, the more difficult it can be to detect cancer on mammograms. Many state regulations have been enacted—and more proposed—requiring health providers to tell women if their mammogram shows their breasts are dense.
- How can radiologists detect breast cancer more accurately?
Research suggests having radiologists do diagnostic workups of some of their own recalled cases can help improve accuracy.
- Wall Street Journal shines light on our patient researchers
As patients assume their groundbreaking role in breast cancer research at KPWHRI, the national press takes notice.
- Getting to Goldilocks: ‘Just right’ breast screening
For Breast Cancer Awareness Month, Dr. Diana Buist tells how Kaiser Permanente research helps women and their doctors decide if, when, and how to screen.
- Lemonade from lemons: Breast cancer group gains momentum
Group Health believes women with breast cancer need their own support group. Thanks to a grant from the Group Health Foundation’s Partnership for Innovation, the Lemonade group was born.
- Recently using some birth control pills may raise breast cancer risk
Women who recently used birth control pills containing high-dose estrogen and a few other formulations had an increased risk for breast cancer, whereas women using some other formulations did not, according to a report about Group Health patients published in Cancer Research, a journal of the American Association for Cancer Research.
- Digital mammograms have raised costs with only small health benefits
The trend toward digital mammograms was given a mixed report card in the study Benefits, Harms, and Costs for Breast Cancer Screening After U.S. Implementation of Digital Mammography e-published on May 28 in the Journal of the National Cancer Institute.
Kaiser Permanente Washington Health Research Institute for:
Kaiser Permanente Washington Health Research Institute
1730 Minor Ave, Suite 1360Seattle, WA 98101-1466 Phone: 206-287-2900
Fax: 206-287-2871
Contact us
Sign up for our newsletter
Get directions
Policy on Conflict of Interest
Nondiscrimination Notice and Language Access Services
Land Acknowledgment
Our Seattle offices sit on the occupied land of the Duwamish and by the shared waters of the Coast Salish people, who have been here thousands of years and remain. Learn about practicing land acknowledgment.