- Our Research
- Research Areas
- Addictions
- Aging & Geriatrics
- Biostatistics
- Cancer
- Cardiovascular Health
- Child & Adolescent Health
- Chronic Illness Management
- Health Informatics
- Health Services & Economics
- Healthy Communities
- Medication Use & Patient Safety
- Mental Health
- Obesity
- Social Determinants of Health
- Vaccines & Infectious Diseases | COVID-19
- Our Scientists
- Collaborate with Us
- Our Publications
- Research Funding Sources
- Research Areas
- News and Events
- Get Involved
- About Us
- Live Healthy
All Articles on Screening
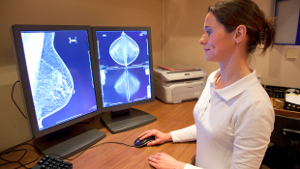
- Some women with dense breasts may not need extra screening
A Breast Cancer Surveillance Consortium study involving Group Health shows that density shouldn’t be the only factor when considering additional screening.
- News release: Home tests and automated reminders cut colon cancer screening costs
With Kaiser Permanente colleagues, Group Health finds cost savings for two years.
- Home tests and automated reminders cut colon cancer screening costs
With Kaiser Permanente colleagues, Group Health finds cost savings for two years.
- Our research made news in 2014
Here’s our list of top 10 research stories of 2014—plus links to the news reports they inspired.
- GHRI names 10 new Group Health clinical associates
The appointment recognizes clinical and administrative colleagues across Group Health who provide invaluable support for the organization’s research.
- Wall Street Journal shines light on our patient researchers
As patients assume their groundbreaking role in breast cancer research at KPWHRI, the national press takes notice.
- Getting to Goldilocks: ‘Just right’ breast screening
For Breast Cancer Awareness Month, Dr. Diana Buist tells how Kaiser Permanente research helps women and their doctors decide if, when, and how to screen.
Kaiser Permanente Washington Health Research Institute for:
Kaiser Permanente Washington Health Research Institute
Phone: 206-287-2900Fax: 206-287-2871
Contact us
Sign up for our newsletter
Policy on Conflict of Interest
Nondiscrimination Notice and Language Access Services
Land Acknowledgment
Our Seattle offices sit on the occupied land of the Duwamish and by the shared waters of the Coast Salish people, who have been here thousands of years and remain. Learn about practicing land acknowledgment.