10 things you can do to prevent devastating falls

A new study shows we know how to stop the leading cause of injury among older people, writes Dr. Eric B. Larson. All we have to do is use that knowledge.
by Eric B. Larson, MD, MPH, Kaiser Permanente Washington Health Research Institute (KPWHRI) executive director, and Kaiser Foundation Health Plan of Washington vice president for research and health care innovation
When my mother was in her late fifties, she had a series of mishaps, beginning with a fall at an outdoor wedding in Montana. Her heel got caught in a gopher hole and down she went, fracturing her ankle. Over the next five years she suffered five more broken bones related to falls—fractures of her hip, wrist, elbow, and each kneecap.
My mother had osteoporosis, a fairly common condition of aging that weakens your bones and can lead to crippling disability. Her doctor prescribed various drug treatments, but most caused bad side effects and had to be stopped.
One recommendation, however, made a big difference. He advised her to start a daily habit of walking and leg-lifting exercises. She followed his advice and after that, the fractures stopped. She wasn’t “cured” of osteoporosis. In fact, her bones did get thinner as she aged, albeit probably slower than without any therapy. But as exercise improved her strength and balance, she quit falling—and so she quit breaking bones!
My mother lived to age 97. Although she needed a wheelchair at times and some assistance for the last two years of her life, she spent most of her older years free to garden, travel, enjoy her grandchildren and a good long life. By avoiding falls and injuries, she avoided the crippling disability that affects so many older people. Falls are the leading cause of both fatal and nonfatal injuries in people aged 65 and older.
Study shows we have the power to stop falls now
I like to tell my mother’s story because it illustrates the power older people have to prevent falling—and thus lead longer, more active, and fulfilling lives. And now comes a comprehensive study, Comparisons of Interventions for Preventing Falls in Older Adults—A Systematic Review and Meta-analysis, published November 7, 2017 in the Journal of the American Medical Association that describes how health care providers can support their patients in doing just that.
Led by Andrea C. Tricco, PhD, of the University of Toronto, researchers reviewed 283 randomized clinical trials involving more than 159,000 participants. They found mountains of evidence that interventions to prevent falls really work—especially those recommending: 1) exercise, and 2) help for poor vision. The team also found that older people do best when their health care teams tailor fall-prevention advice to individual patients’ needs.
And unlike so many research studies, Dr. Tricco’s team did not conclude, “more research is needed.” On the contrary, we already know plenty about how to prevent falls! In an editorial accompanying the Tricco article, I’m challenging everybody in health care to share that knowledge well and broadly, and encouraging everyone to take steps now to stop falls from happening. Using our information, we can take an activist, enlightened approach to aging!
In that spirit, here are 10 fall-prevention tips I’ve gleaned from our research at KPWHRI and elsewhere. I hope they help you and your loved ones stay safe and healthy for many years to come:
- Be physically active.
Regular (ideally daily) exercise, such as walking, swimming, or bicycling can help you build muscle strength, balance, and reduce fatigue. Activities like yoga, Pilates, and tai chi can also help. Avoid long periods of sitting; interrupt your sedentary time with frequent walks and stretching. And if illness or injury slows you down, make rehabilitation exercises a top priority. Resistive exercise with light weights or bands can help maintain or build muscle strength, which will otherwise decline with age. - Check your vision.
Eyesight usually deteriorates as you age and, in some cases, the decline may not even be noticed. This puts you at risk for falling over things you may not see. That’s why people over age 65 should have regular, comprehensive, dilated eye exams, and keep prescription eyeglasses up-to-date. Such exams may be important to check for certain eye diseases that can lead to severe vision problems if left untreated. - Wear proper shoes or slippers.
Research conducted by KPWHRI and the University of Washington found that the safest shoes have laces or Velcro fasteners, adequate heel support, and non-slip soles. (Translation: Wear a good “tennis shoe.”) The highest risk for falls comes from walking around barefoot or in stocking feet—even indoors. Also, avoid high heels. - Check your medications—especially sleeping pills.
Talk to your doctor if you have dizziness or fatigue. The problem might be linked to certain medications. Drugs for high blood pressure and chronic pain often cause balance problems, leading to falls. Antidepressants, anti-psychotics, anti-anxiety and sleeping medications—especially benzodiazepine tranquilizers—can also be problematic. As I sometimes tell my patients, “Nobody ever died because they could not sleep, but I’ve seen people who broke their hips because their sleeping pills made them wobbly,” leading to premature disability and death. - Get the right equipment.
Use canes or walkers if you need them. Don’t let vanity get in your way. Think of such devices as a sign of your activist, intelligent approach to aging well. - Be safe in the bathroom.
Many falls happen around the toilet, bathtub, and shower. Install and use handholds. Get a shower chair if you’re unsteady standing for long periods. Keep a pair of nonslip slippers with good soles beside your bed to wear when nature calls. - Avoid too much alcohol.
Some of the most tragic falls I’ve seen have involved older patients who had too much alcohol, usually around dinner or while watching TV. Be careful when drinking, to avoid tipsiness—a sign that your balance and reactions are impaired, which increases your chance of falling and reduces your ability to recover if you start to go down. Also beware of interactions between drinks and prescription medications that might make you unsteady. - Eliminate household hazards.
Get rid of loose electrical cords and throw rugs. Avoid slippery floors and icy surfaces. Make sure rooms and passageways are well lit. Use night lights. - Consider vitamin D.
Ask your doctor about this supplement, which may improve muscle strength, balance, and reduce falls. It may especially benefit people living in northern latitudes where less sunlight reduces the body’s ability to use vitamin D to maintain bone strength, thereby contributing to more osteoporosis. - Talk to your health care team about your risk.
As Dr. Tricco’s recent study shows, those who get tailored advice from their care providers often do best at preventing falls. This may be especially important if you haven’t exercised much recently but want to get started now. If so, you could be at greater risk for falls initially, but with care, you can become more physically active and you will benefit. Your provider may also recommend changes related to your medications, your vision, potential hazards in your home, and more.
Live Healthy: Top Topics
Enlightened Aging

Proactive boomers will ‘choose their own adventure’ in growing old
In an excerpt from his new book, Enlightened Aging, Dr. Eric B. Larson encourages his generation to build reserves for a long life ahead.
Read it in Enlightened Aging.
Research on healthy aging
ACT study
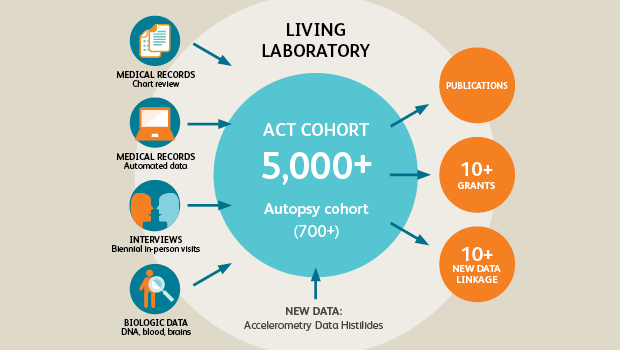
ACT study: Long-running study of aging examines changes in Kaiser Permanente patients over time
Drs. Larson and Crane co-lead Kaiser Permanente-University of Washington collaboration learning how to promote healthy aging.


