Study shows benefits of 3D mammography
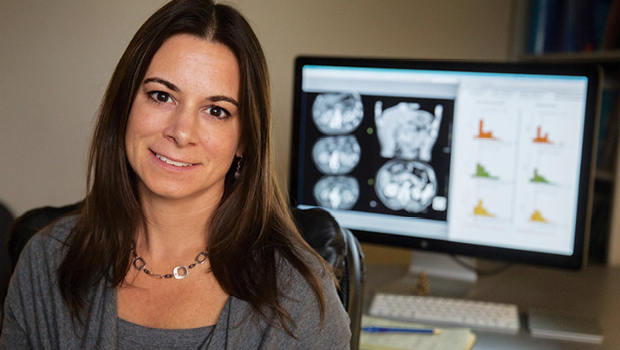
Digital breast tomosynthesis reduced patient recalls with no change in cancer detection, study shows.
Radiologists quickly learn to read 3D mammography more accurately than they read standard 2D mammograms, a first-of-its-kind study led by a Kaiser Permanente Washington Health Research Institute (KPWHRI) investigator has found.
Published recently in Radiology, the study was led by Diana Miglioretti, PhD, KPWHRI senior investigator and dean’s professor of biostatistics in the University of California Davis Department of Public Health Sciences. Collaborators included KPWHRI biostatistician Linn Abraham, MS, and Senior Investigator and Director of Research and Strategic Partnerships Diana S.M. Buist, PhD, MS. The team found that radiologists who interpret traditional mammograms, which are two-dimensional, required little start-up time for transitioning to reading digital breast tomosynthesis (DBT), also called 3D mammography, with improved screening accuracy.
Researchers found radiologists recalled patients for additional testing at a lower rate on DBT than they did on 2D mammography, without sacrificing cancer detection. A patient may be recalled if a suspicious finding on the screening examination requires follow-up imaging and possibly biopsy to determine if it is cancer. Three-dimensional views taken as part of a DBT screening help the radiologist confirm that some findings on 2D images are not cancer, so fewer patients have to be recalled. These improvements were seen regardless of the patient’s breast density.
“We found that patients with or without dense breasts benefit from lower recall rates with 3D mammography and there is no trade off with cancer detection,” Dr. Miglioretti said. “In fact, we were surprised to find that improvements in recall rates were larger in women without dense breasts.”
Broad range and large number of radiologists sampled
The study included data from 104 radiologists from 53 facilities in five U.S. states, collected by the Breast Cancer Surveillance Consortium (BCSC) to evaluate whether radiologists experience a learning curve for 3D mammography interpretive performance. Kaiser Permanente Washington is one of the health care systems that contributes data to the BCSC. The study is the largest of its kind and represented a broad range of radiology centers and providers. It is novel because it tracked radiologists’ performance over time as they transitioned from digital mammography to DBT.
DBT takes multiple X-ray images of each breast from many angles which are then computer assembled into a three-dimensional image of the breast that the radiologist can scroll through. The U.S. Food and Drug Administration requires only eight hours of additional training for qualified radiologists to be able to interpret DBT studies. Researchers wondered if a learning curve was associated with the interpretive performance of this new technology and if any improvements are sustained by radiologists over time.
“We found both breast imaging subspecialists and general radiologists improved their screening performance when they switched from 2D to 3D mammography,” said Dr. Miglioretti. “These improvements were sustained for at least two years after adoption of the new technology.” This finding in particular was noted as important in an accompanying editorial from Regina Hooley, MD, of Yale School of Medicine.
Most women in the United States do not have their mammograms interpreted by a breast imaging subspecialist, nor do they have access to academic medical centers. The study evaluated radiologists with a mix of experience at both academic and nonacademic facilities. Both breast imaging subspecialists and general radiologists improved their interpretive performance quickly after adopting DBT, with lower recall rates and similar cancer detection rates as for digital mammography.
At the end of her editorial, Dr. Hooley concludes: "This important study by Miglioretti et al confirms that the major benefit of DBT in the screening setting within the United States is the significant reduction in recall rate, with no change in cancer detection rate. The screening recall rate was most improved among non–breast imaging specialist radiologists and in women with nondense breasts. Cancer detection rates were maintained and trended slightly higher, signifying improved accuracy of DBT screening, without requiring a significant radiologist learning curve.
"Further advances in DBT technology, perhaps coupled with careful attention to radiologist training, will likely continue to improve the accuracy and performance of screening mammography," Dr. Hooley states.
Other collaborating researchers were Christoph I. Lee, MD, MBA, University of Washington; Sally Herschorn, MD, and Brian L. Sprague, PhD, University of Vermont; Louise M. Henderson, PhD, UNC Chapel Hill; Anna N.A. Tosteson, ScD, Dartmouth University; and Karla Kerlikowske, MD, UCSF.
This research was supported by a Patient-Centered Outcomes Research Institute Program Award (PCS-1504-30370). Data collection was additionally supported by the Agency for Healthcare Research and Quality (R01 HS018366-01A1); National Cancer Institute (P01CA154292, U54CA163303); and the University of Vermont Cancer Center (Lake Champlain Cancer Research Organization grant 032800). Dr. Lee was supported by the American Cancer Society (126947-MRSG-1416001CPHPS).
Based on an original news release from UC Davis.
Research findings

Using breast MRI after cancer may lead to unneeded biopsies
A Kaiser Permanente-led BCSC study is among the largest to evaluate adding MRI surveillance for breast cancer survivors.
healthy findings blog
What to expect after a screening breast MRI vs. mammography alone
Diana Buist and BCSC find screening MRI leads to more biopsies, finding fewer cancers, regardless of personal history of breast cancer: JAMA Internal Medicine.
Researcher profile

Why does Diana Miglioretti study the biostatistics of cancer screening?
Family history sparks interest for KPWHRI senior investigator, UC Davis professor, and co-leader of the BCSC.
Read it in News and Events.


