NIH-Moderna COVID-19 vaccine receives FDA Emergency Use Authorization

The investigational vaccine that KPWHRI’s team first tested shows an efficacy rate of about 94% as research continues
The U.S. Food and Drug Administration approved Dec. 18, 2020, an emergency use authorization of the COVID-19 vaccine known as mRNA-1273, co-developed by the Cambridge, Massachusetts-based biotechnology company Moderna Inc., and the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health.
The FDA's decision follows the release of preliminary results from a phase 3 trial, which found the vaccine was safe and effective at preventing symptomatic COVID-19 in adults. A full review of the data has now confirmed these earlier findings, with a vaccine efficacy rate of 94.1%. Kaiser Permanente Washington Health Research Institute (KPWHRI) was one of about 100 sites participating in the trial.
Additional evidence of its benefits were reported Dec. 3, 2020, in a letter in the New England Journal of Medicine co-authored by Lisa A. Jackson, MD, MPH, senior investigator at KPWHRI. Based on data from the phase 1 clinical trial led by Dr. Jackson and her team, investigators found that the mRNA vaccine continued to provide a significant immune response 119 days after first vaccination and 90 days after second vaccination in 34 healthy adults.
The mRNA-1273 vaccine is the second vaccine to receive an emergency use authorization from the FDA. The developers of the other vaccine, Pfizer and BioNTech, were granted Emergency Use Authorization by the FDA a week ago. Kaiser Permanente has participated in clinical trials of that vaccine in California, and Americans began receiving shots of it earlier this week. It is widely anticipated that injections of the mRNA-1273 vaccine will begin in the next few weeks.
The vaccine research team at KPWHRI launched the phase 1 trial of the mRNA-1273 vaccine candidate in March 2020. It combines Moderna’s mRNA (messenger RNA) delivery platform with the stabilized SARS-CoV-2 spike immunogen (S-2P) developed by NIAID scientists. KPWHRI's work on the phase 1 and phase 3 trials of the NIAID-Moderna vaccine is ongoing.
The interim analysis of the phase 3 data, released Nov. 16, comprised 95 cases of symptomatic COVID-19 among volunteers. The independent NIH-appointed Data Safety Monitoring Board (DSMB) overseeing the phase 3 trial reported that the vaccine candidate was safe and well-tolerated and noted a vaccine efficacy rate of 94.5%. The findings are statistically significant, meaning they are likely not due to chance. Of the cases, 90 occurred in the placebo group and 5 occurred in the vaccinated group. There were 11 cases of severe COVID-19 out of the 95 total, all of which occurred in the placebo group.
Two weeks later, an analysis of the phase 3 data, released Nov. 30, identified 196 cases of symptomatic COVID-19 among volunteers, with 185 of these from the group that had received a placebo, resulting in a point estimate of vaccine efficacy of 94.1%.
“Our research team is thrilled with the results and tremendously grateful to the thousands of study volunteers who have stepped forward to help all of society in our global fight against the virus,” said Dr. Jackson. “As our work continues, I also want to acknowledge my colleagues at the other research sites and in our vaccine research unit at Kaiser Permanente Washington, who have been working tirelessly since January to bring us to this point. With these results, we can feel confident that our continued work on the front lines through the pandemic will ultimately help save lives around the world.”
Steps in development
The NIAID-Moderna vaccine candidate transitioned from early development with NIAID to the Biomedical Advanced Research and Development Authority (BARDA), part of the Department of Health and Human Services Office of the Assistant Secretary for Preparedness and Response, for advanced development and manufacturing support, to meet the federal government’s Operation Warp Speed (OWS) goals.
The phase 3 vaccine efficacy trial, known as COVE, was begun under OWS, a multi-agency collaboration led by HHS and the Department of Defense that aims to accelerate the development, manufacturing and distribution of medical countermeasures for COVID-19. The Accelerating COVID-19 Therapeutic Interventions and Vaccines (ACTIV) partnership advised on the trial protocol design and endpoints to ensure a harmonized approach across multiple vaccine efficacy trials. The partnership brings NIH together with other HHS agencies and government partners and representatives from academia, philanthropic organizations, and numerous biopharmaceutical companies to develop a coordinated research strategy for prioritizing and speeding development of the most promising treatments and vaccines.
More than 30,000 participants are now participating in the study, which launched on July 27, 2020, after results from earlier stage clinical testing indicated that the vaccine candidate is well-tolerated and immunogenic. Recognizing the disproportionate impact of the epidemic on underrepresented minority populations, investigators worked with community engagement partners to enroll a diverse pool of participants. Of the trial volunteers, 37% are from racial and ethnic minorities.
The COVE trial is sponsored by Moderna. BARDA and NIAID are providing funding and technical support for the trial. A total of 25 NIH-funded COVID-19 Prevention Network sites enrolled participants in the trial.
The co-principal investigators for the study are Hana M. El Sahly, MD, principal investigator of the NIAID-funded Infectious Diseases Clinical Research Consortium site at Baylor College of Medicine in Houston; Lindsey R. Baden, MD, principal investigator of the NIAID-funded Harvard HIV Vaccine Clinical Trials Unit at Brigham and Women’s Hospital in Boston; and Brandon Essink, MD, principal investigator and medical director of Meridian Clinical Research.
More detailed information about the trial, including more comprehensive data, will be available in a forthcoming report. For more information about the trial, visit clinicaltrials.gov and search identifier NCT04470427.
Volunteering for COVID-19 vaccine trials
Kaiser Permanente Washington’s vaccine research group has a registry of Seattle-area people who want to be considered to participate in possible trials of investigational vaccines for COVID-19 at Kaiser Permanente Washington in Seattle: corona.kpwashingtonresearch.org.
The COVID-19 Prevention Trials Network has a volunteer screening registry of people nationwide who are interested in participating in a broader range of vaccines and other preventive treatments at various research facilities in Seattle and around the country: coronaviruspreventionnetwork.org.
About the COVID-19 Prevention Network
The COVID-19 Prevention Network (CoVPN) was formed by the National Institute of Allergy and Infectious Diseases (NIAID) at the U.S. National Institutes of Health to respond to the global pandemic. Through the CoVPN, NIAID is leveraging the infectious disease expertise of its existing research networks and global partners to address the pressing need for vaccines and antibodies against SARS-CoV-2. CoVPN will work to develop and conduct studies to ensure rapid and thorough evaluation of vaccines and antibodies for the prevention of COVID-19. The CoVPN is headquartered at the Fred Hutchinson Cancer Research Center. For more information about the CoVPN, visit: coronaviruspreventionnetwork.org.
About the National Institute of Allergy and Infectious Diseases
NIAID conducts and supports research — at NIH, throughout the United States, and worldwide — to study the causes of infectious and immune-mediated diseases and to develop better means of preventing, diagnosing, and treating these illnesses. News releases, fact sheets, and other NIAID-related materials are available on the NIAID website.
About the National Institutes of Health
NIH, the nation's medical research agency, includes 27 institutes and centers and is a component of the Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit the NIH website.
About Kaiser Permanente Washington Health Research Institute
Kaiser Permanente Washington Health Research Institute (KPWHRI) improves the health and health care of Kaiser Permanente members and the public. The Institute has conducted nonproprietary public-interest research on preventing, diagnosing, and treating major health problems since 1983. Government and private research grants provide our main funding. Follow KPWHRI research on Twitter, Facebook, LinkedIn, or YouTube. For more information, go to: www.kpwashingtonresearch.org.
This story was first published on Nov. 16, 2020. It was updated on Dec. 18, 2020, to record the FDA’s granting of an Emergency Use Authorization for the mRNA-1273 vaccine. It had previously been updated on Dec. 7, 2020, to include information about Moderna’s application for emergency use of its mRNA-1273 vaccine as well as to report on new findings. For the original Nov. 16 version, please click here to download a PDF. For the Dec. 7 version, please click here.
news

Janssen phase 3 COVID-19 vaccine trial to begin at KPWHRI
The institute is participating in NIAID tests of Moderna and Johnson & Johnson vaccines.
News
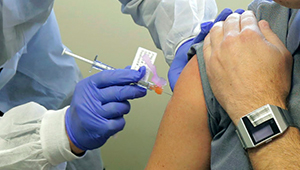
COVID-19 vaccine well tolerated, generates immune response
National Institute of Allergy and Infectious Diseases-sponsored phase 1 trial tested mRNA vaccine.
research
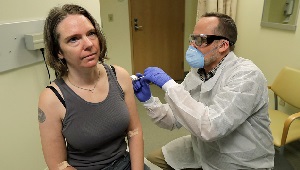
Kaiser Permanente launches first coronavirus vaccine trial
On March 16, 4 volunteers received an injection of an mRNA vaccine for COVID-19 in an NIH-funded trial in Seattle.
Research
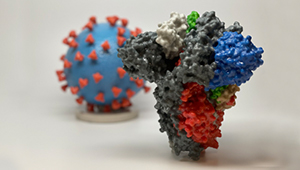
COVID-19 pandemic research at KPWHRI
Having long tracked infectious diseases and tested vaccines, KPWHRI now focuses on the novel coronavirus.



