CVD risk calculation: Can smaller clinics break through?
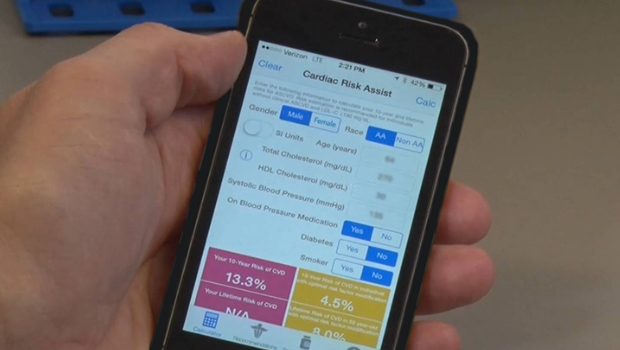
A primary care doctor calculates a patient’s risk of cardiovascular disease.
KPWHRI researchers uncover the obstacles faced by smaller practices when integrating CVD risk calculators into primary care
American Heart Month rolls around every February, shining a valuable spotlight on the heart-healthy steps people can take to prevent cardiovascular disease (CVD). Of course, turning these recommendations into lasting changes in diet, lifestyle, and treatment takes much more than a well-publicized annual campaign. And one key motivating factor may be missing for many people: a clear understanding from their doctor of their cardiovascular risk.
Resistance to risk calculators
National guidelines recommend primary care physicians use evidence-based calculators to estimate patients’ risk of developing CVD. These calculators — such as the one promoted by the American College of Cardiology/American Heart Association — provide risk estimates and treatment recommendations based on a patient’s age, gender, race, cholesterol levels, blood pressure, and whether the person has diabetes or smokes.
Despite these recommendations, uptake of CVD risk calculators in primary care has been slow, with a national study finding that only 41% of primary care physicians calculate CVD risk in the clinic. This study and others have identified common barriers to adopting these tools, such as the perception that use of calculators takes up too much time and that explaining absolute CVD risk to patients is too difficult. The barriers for smaller clinics may be particularly daunting, given that these practices typically have fewer resources and staff to implement risk calculators and other innovations. However, previous studies have not explored this.
To help fill this gap, researchers at Kaiser Permanente Washington Health Research Institute (KPWHRI) and colleagues investigated the unique barriers to implementing CVD risk calculators in smaller primary care clinics. Their findings have now been published in the American Journal of Preventive Medicine.
“With this publication, we sought to facilitate improvements to patient care by sharing common barriers to implementing the CVD risk calculator into small to medium primary care clinics,” says KPWHRI Research Specialist Erika Holden, who was part of the team that assembled and analyzed the study data.
Harvesting data from Healthy Hearts NW
The research team analyzed data from the Healthy Hearts Northwest (H2N) trial, which KPWHRI researchers led as part of the EvidenceNOW: Advancing Heart Health in Primary Care initiative funded by the Agency for Healthcare Research and Quality. H2N aimed to help smaller primary care practices adopt evidence-based approaches to improving cardiovascular care outcomes, including integrating a CVD risk calculator into patient visits.
The H2N trial included 209 primary care clinics in Washington, Oregon, and Idaho with 10 or fewer primary care providers. All the enrolled clinics worked with a dedicated practice “coach” at their locations over 15 months. Half of the clinics were also randomized to receive an educational outreach visit for members of their care team, and 44 clinics participated.
These outreach visits, facilitated by physician educators through webinars, focused on 3 main areas: (1) CVD risk calculation guidelines, (2) shared decision-making with patients, and (3) when to initiate statin medications. As part of these discussions, the outreach educators asked about potential barriers or objections to the use of a CVD risk calculator in the clinic. Structured notes from these discussions were the basis of KPWHRI’s new analysis.
Common themes, unique insights
After identifying the barriers to CVD risk calculation in the structured notes, the research team sorted these barriers into 13 distinct categories, ranked from most to least common. The 5 most common barriers were:
- Time constraints to using a calculator, or competing demands (52% of the clinics)
- Limitations to accessing a calculator or the necessary information to use a calculator (50%)
- No or minimal buy-in from clinicians or staff to use or promote a calculator (43%)
- Reported patient fear of side effects from statin medications or patient dislike of taking medications per guidelines (39%)
- Lack of documented clinic workflow for using a calculator (36%)
Some of the 13 barriers — such as time constraints — had been identified in earlier studies that also included larger practices. However, several of the barriers cited by smaller clinics were new, including patients’ concerns about statins (39%), lack of documented workflows (36%), clinic staffing issues (9%), concerns about patients’ out-of-pocket costs (7%), and inadequate communication within the team (5%).
As a next step in addressing these barriers, the researchers mapped all 13 barriers to the Consolidated Framework for Implementation Research (CFIR), a conceptual framework of key domains that can inform the adoption of health service innovations. Of the top 5 barriers to implementing CVD risk calculation in the study, 4 aligned with the “Inner Setting” domain. This suggests, say the researchers, that internal resources, time, and availability of clinical team members to implement CVD risk calculation should be considered when evaluating the strategy and feasibility of future interventions for smaller practices.
Recognizing the barriers faced by smaller clinics can open the door to more tailored interventions, says KPWHRI Senior Research Associate Leah Tuzzio, MPH, who led the study. If time constraints are a main concern, for example, an intervention might integrate CVD risk calculation into existing workflows or add technical tools that auto-fill information from the electronic health record into the calculator, allowing providers to efficiently calculate CVD risk. The options for innovation are many.
“With this information, my hope is that researchers can study how to tailor interventions to the unique barriers that small clinics face,” Tuzzio says.
By Sophie Ramsey
Interested in learning more about integrating CVD risk calculation into primary care? In the video below, Christopher Dodd, MD, MS, shares how he uses a risk calculator to help patients improve their heart health (the patient-doctor encounters are simulations).
researchers
,
,
James D. Ralston, MD, MPH
Senior Investigator
research into action

Healthy Hearts Northwest helps small clinics improve care
A new study shows how a little supplemental support can result in big gains, especially in managing patients’ blood pressure.
improving care

Partnership with rural-health experts aims to improve heart care
Healthy Hearts Northwest is helping patients receive better care for cardiovascular conditions thanks to collaborators like Dr. L.J. Fagnan.


