Improving Chronic Illness Care
The Chronic Care Model
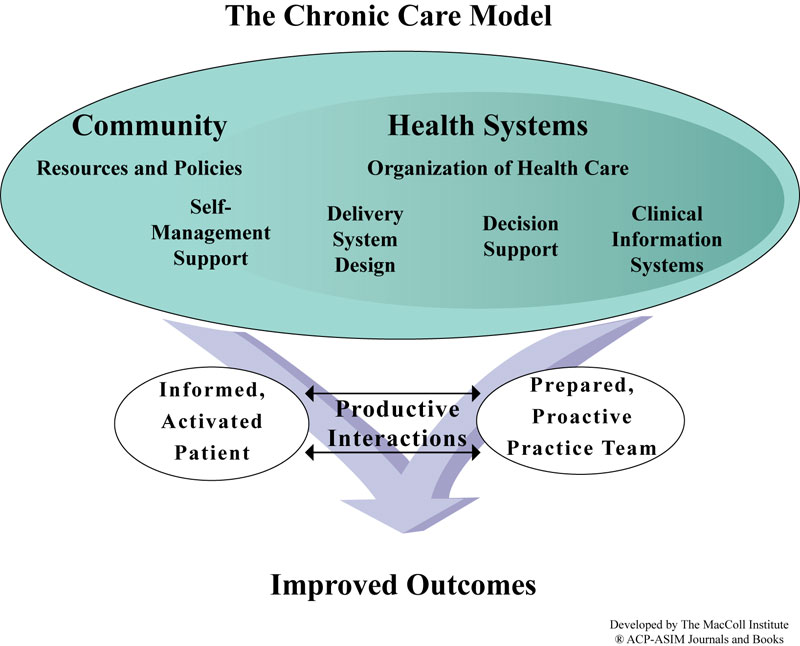 The Chronic Care Model (CCM) identifies the essential elements of a health care system that encourage high-quality chronic disease care. These elements are the community, the health system, self-management support, delivery system design, decision support and clinical information systems. Evidence-based change concepts under each element, in combination, foster productive interactions between informed patients who take an active part in their care and providers with resources and expertise.
The Chronic Care Model (CCM) identifies the essential elements of a health care system that encourage high-quality chronic disease care. These elements are the community, the health system, self-management support, delivery system design, decision support and clinical information systems. Evidence-based change concepts under each element, in combination, foster productive interactions between informed patients who take an active part in their care and providers with resources and expertise.
The Chronic Care Model can be applied to a variety of chronic illnesses, health care settings, and target populations. The bottom line is healthier patients, more satisfied providers, and cost savings.
linked resources
- Chronic Care Model change concepts
- Assessment of Chronic Illness Care (PDF)
- Patient Assessment of Chronic Illness Care - 20-item version (PDF)
- Patient Assessment of Chronic Illness Care - original version (PDF)
- How the Chronic Care Model was developed
For citations concerning the evolution of the Chronic Care Model, please reference this journal article: Wagner EH. Chronic disease management: what will it take to improve care for chronic illness? Eff Clin Pract. 1998;1:2-4. (The Chronic Care Model image first appeared in its current format in this article.)
The Care Coordination Model & Toolkit
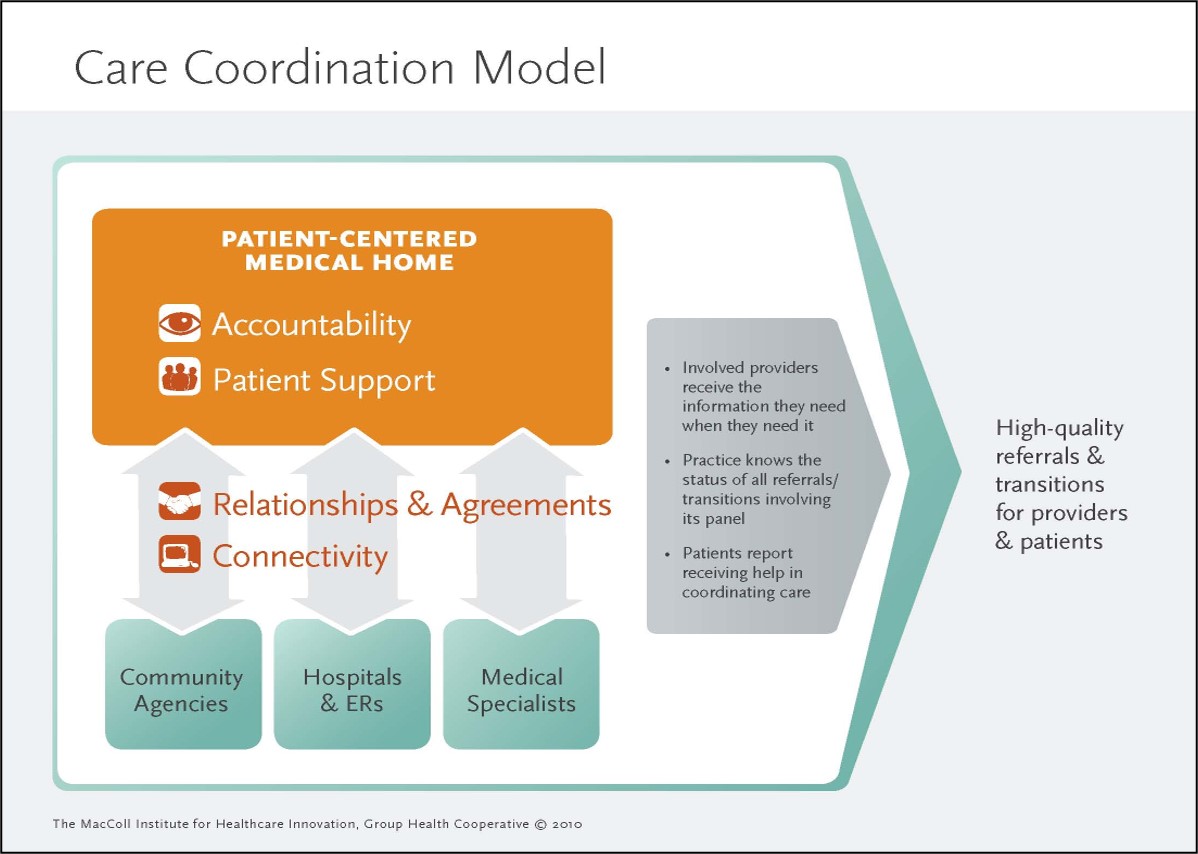 The Care Coordination Model looks at care coordination from the perspective of a patient-centered medical home (PCMH). It considers the major external providers and organizations with which a PCMH must interact – medical specialists, community service agencies, and hospital and emergency facilities – and summarizes the elements that contribute to successful referrals and transitions.
The Care Coordination Model looks at care coordination from the perspective of a patient-centered medical home (PCMH). It considers the major external providers and organizations with which a PCMH must interact – medical specialists, community service agencies, and hospital and emergency facilities – and summarizes the elements that contribute to successful referrals and transitions.
The Care Coordination Model and accompanying toolkit are designed for clinics, practices, and health systems focused on improving care coordination by transforming the way they manage patient referrals and transitions.
Linked resources
- Care Coordination Model (JPEG)
- Reducing Care Fragmentation: A Toolkit for Coordinating Care (PDF)
- Reducing Care Fragmentation: Executive Summary (PDF)
- Reducing Care Fragmentation: A Presentation on Coordinating Care (PPT)
- Presentation: Key Changes and Resources for Care Coordination (PPT)
Suggested citation: Reducing Care Fragmentation: A Toolkit for Coordinating Care. (Prepared by Kaiser Permanente’s MacColl Institute for Healthcare Innovation, supported by The Commonwealth Fund), April 2011.
Using our materials in
your work
The MacColl Center encourages the
non-commercial use or adaptation of the materials we develop. With the exception of the Chronic Care Model image at left, all other materials provided here are publicly available, free of cost and copyright protected.
contact us
Please email us at maccoll@kp.org for help finding additional tools from Improving Chronic Illness Care.
Our other websites
The MacColl Center's funding for Improving Chronic Illness Care ended in 2011, but our work to improve care with a patient-centered, team-based approach has continued. To access some of our more recent tools and resources, please visit these websites:
Assessments
- Assessment of Chronic Illness Care (ACIC)
- Patient Assessment of Chronic Illness Care (PACIC - 20 item)
- Patient Assessment of Chronic Illness Care (PACIC - original)
- Patient-centered Medical Home Assessment (PCMH-A)



