Cataract surgery linked with lessened dementia risk
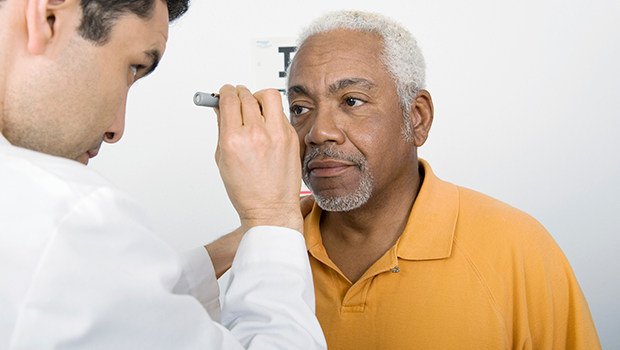
Study in JAMA Internal Medicine finds cataract surgery associated with 30% lower risk of dementia in aging population
Cataracts affect most older adults at risk for Alzheimer’s disease and other types of dementia. Now, researchers are finding strong evidence that having surgery to remove cataracts is associated with a lower risk of developing dementia.
The Adult Changes in Thought (ACT) Study is a long-standing, Seattle-based observational study at Kaiser Permanente Washington of more than 5,000 participants older than 65. Based on the longitudinal data of over 3,000 ACT study participants, researchers have now found that individuals who underwent cataract surgery had nearly 30% lower risk of developing dementia from any cause compared with those who did not. This lowered risk persisted for at least a decade after surgery. Cataract surgery was also associated with lower risk of Alzheimer’s disease dementia specifically. The results were reported Dec. 6 in JAMA Internal Medicine.
Lead researcher Cecilia S. Lee, MD, MS, associate professor at the University of Washington School of Medicine, said the observational study took into account a number of potential confounders (variables that could have affected the findings), yet still yielded a strong association.
“This kind of evidence is as good as it gets in epidemiology,” Lee said. “This is really exciting because no other medical intervention has shown such a strong association with lessening dementia risk in older individuals.”
The mechanisms by which cataract surgery and lessened dementia risk are associated was not determined in this study. Researchers hypothesize that people may be getting higher-quality sensory input after cataract surgery, which might have a beneficial effect in reducing the risk of dementia.
“These results are consistent with the notion that sensory input to the brain is important to brain health,” said Eric Larson, MD, MPH, principal investigator of the ACT Study.
Lee said another hypothesis is that, after cataract surgery, people are getting more blue light.
“Some special cells in the retina are associated with cognition and regulate sleep cycles, and these cells respond well to blue light,” she said. “Cataracts specifically block blue light, and cataract surgery could reactivate those cells.”
The study results highlight a strong case for further research on the eye-brain connection in dementia. Previous studies have shown a strong link between other retinal diseases, such as age-related macular degeneration, and the development of Alzheimer’s disease and dementia. In the current study, participants undergoing vision-improving cataract surgery had lower risk of developing dementia. Further understanding of the connection between the aging eye and brain may offer insights and potential therapies to slow or prevent age-related dementia.
The study
Researchers tracked participants diagnosed with a cataract or glaucoma but who did not have dementia at the time they volunteered for the study. Participants also did not have cataract surgery at the time of enrollment. Participants were evaluated every 2 years for cognitive abilities based on the Cognitive Abilities Screening Instrument, which scores in a range from 0 to 100. Participants with scores less than 85 had further neurological tests.
During follow-up of 3,038 participants (7.8 years of follow-up per person on average), 853 people developed dementia, with 709 cases of Alzheimer’s disease. Approximately half of the participants (1,382 individuals or 45%) had cataract surgery. Analysis for risk of developing dementia showed that participants who had undergone cataract surgery in either eye were about 30% less likely to develop any form of dementia for at least 10 years after their surgery.
Analysis was adjusted for an extensive list of factors including health-related confounders. Cataract surgery could appear to have a protective effect due to a healthy patient bias, where participants who underwent cataract surgery might have been healthier and at lower dementia risk. Researchers performed analyses to account for this and several other types of potential bias but still found strong associations when these factors were accounted for.
Researchers excluded eye surgeries in the 2 years prior to dementia diagnosis to rule out the possibility that people with cognitive decline prior to dementia diagnosis may have been less conscious of vision issues, and thus less likely to have undergone cataract surgery. Even with this group excluded, the researchers found lower risks of dementia associated with cataract surgery.
As another control, participants were also evaluated for a possible link between another type of eye surgery (glaucoma surgery) and dementia. In this case, no association was found.
The study was a community-based, prospective cohort study with more than 23,000 person-years of follow-up. More than 98% of the ACT cohort were seen at least once by eye care clinicians, with an average of 27 encounters. Dementia diagnoses were made by a panel of experts using research criteria.
Study limitations include that results could be explained by unmeasured or residual confounding factors, as in any observational study. There could be coding errors for cataract diagnosis. Only the participant’s first cataract surgery was evaluated, so researchers don’t know whether subsequent surgeries impacted dementia risk. The majority of the study population was white, and it is unclear if the effect would be observed in all populations.
This has been adapted from a news story on this study by UW Medicine, University of Washington.
ACT Study

Roundup of 3 recent studies on dementia risk
Researchers explore links between hearing loss, military service, and cognitive decline — and look at timeliness of diagnosis.
alzheimer's research
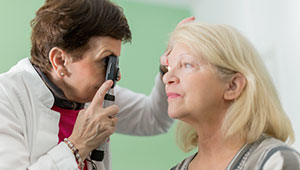
Eye conditions may help screen for Alzheimer’s disease
Age-related macular degeneration, diabetic retinopathy, glaucoma could be new lens on dementia risk.
New funding

Grant of over $55M to boost Alzheimer’s, dementia study
Kaiser Permanente Washington will co-lead an expanded ACT Program to better understand the aging brain.
Research
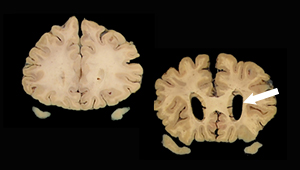
Study evaluates biomarker criteria for Alzheimer’s risk
One-third of people classified as ‘highest risk’ may not develop Alzheimer’s disease, study suggests
Live Healthy

How to lower your risk of dementia
It’s never too late (or too soon) to take preventive steps.


