Roundup of 3 recent studies on dementia risk

Researchers explore links between hearing loss, military service, and cognitive decline — and look at timeliness of diagnosis
As dementia research accelerates, studies are offering new insights into how the body, especially the brain, ages — and how people can age in the healthiest possible ways. Below is a roundup of 3 recent studies based on the Adult Changes in Thought (ACT) Study, a joint project between Kaiser Permanente Washington, University of Washington (UW), and University of California-San Diego that focuses on finding ways to delay or prevent dementia, including Alzheimer's disease, and declines in memory and thinking.
Dementia risk and hearing
The Lancet Commission’s 2020 report suggests that hearing may be especially important to study in terms of dementia risk. A study published Oct. 13 in JAMA Otorhinolaryngology suggests that central auditory processing — or how the brain processes sound — could provide further insight.
In an observational study of 280 older adults without dementia, researchers found that people who performed at intermediate and poor levels on dichotic tests (both ears) were at substantially increased risk of developing dementia during an average of nearly 8 years of follow-up. Dichotic tests measure some aspects of central auditory processing.
Sound perception can be tested with standard audiology testing, where beeps at different frequencies are presented at different volumes to determine thresholds for sound perception. Once speech has been perceived, it needs to be transformed by the brain into language.
This study administered 2 types of hearing evaluations: the standard audiology threshold tests as well as dichotic tests.
In one of the dichotic tests, noise is presented to one ear and a number is presented to the other ear; the participant is asked to say the name of the number. Dichotic tests assess the brain’s ability to manage competing auditory signals and to isolate speech against a background of noise.
Co-senior author Paul Crane, MD, MPH, professor of medicine at UW, said this study suggests that further research on the relationship between hearing and dementia risk should consider adding dichotic tests as part of the measurement.
An important underlying scientific question is what aspect of hearing loss is associated with dementia, said co-senior author Eric Larson, MD, MPH, a senior investigator at Kaiser Permanente Washington Health Research Institute.
Larson said George Gates, MD, professor emeritus of otolaryngology at UW Medicine, was a pioneer in the early research linking dementia to a decline in central auditory processing in midlife.
“This paper is testament to his work,” he said.
Funder: The National Institute on Aging
Military service and dementia
As the number of U.S. veterans over age 65 has grown, researchers want to know whether military service is associated with an increased risk of cognitive decline.
In a study published in Military Medicine Oct. 9, researchers studied 4,370 participants and found no such link. Researchers classified persons as having military employment if their first- or second-longest occupation was with the military. Of the participants, 6% had military employment; of these, 76% were males.
“While our study suggests no overall increase in risk for those with military employment, we still need to better understand how specific experiences that are unique to our veterans may impact risk of cognitive decline and dementia,” said lead author Melinda Power, ScD, associate professor of epidemiology at the George Washington University Milken Institute School of Public Health.
She said veterans can benefit from the same advice given to the general population — stay active, eat well, and actively manage your chronic conditions.
“Heart health is especially important, as what’s good for your heart appears to be good for your brain,” Power said.
Co-authors on the study include Eric Larson and Paul Crane.
Funder: Department of Defense Peer Reviewed Alzheimer’s Research Program
Dementia timely diagnosis
How often do people with dementia or mild cognitive impairment get a timely diagnosis — and are there factors, such as race and educational level, that might affect the timing of this diagnosis?
In an observational study published in the Journal of General Internal Medicine Oct. 13, researchers looked at 4,760 participants with dementia and 1,864 participants with mild cognitive impairment. They evaluated the timing of each participant’s diagnosis in relation to when they first had cognitive scores indicating these conditions. The study team found that only 26% of people with dementia and just 11.4% of people with mild cognitive impairment received a timely diagnosis.
Non-Hispanic Black participants and participants with less than a college degree were significantly less likely to receive a timely diagnosis than non-Hispanic white participants with a college degree. Participants who lived alone were also less likely to receive a timely diagnosis of dementia, though not mild cognitive impairment.
Researchers concluded that targeting resources for timely diagnosis of cognitive impairment to individuals from certain racial and ethnic groups or with lower educational levels, and those living alone, may improve detection and reduce disparities in obtaining timely diagnosis of dementia and mild cognitive impairment.
Lindsey White, PhD, with RTI International in Seattle led the study. Co-authors included Eric Larson.
Funder: The National Institute of Aging
This has been adapted from a news story on this study by UW News, University of Washington.
New funding

Grant of over $55M to boost Alzheimer’s, dementia study
Kaiser Permanente Washington will co-lead an expanded ACT Program to better understand the aging brain.
Research
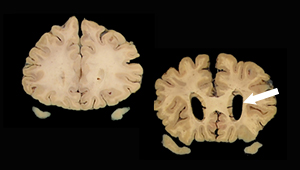
Study evaluates biomarker criteria for Alzheimer’s risk
One-third of people classified as ‘highest risk’ may not develop Alzheimer’s disease, study suggests
Research
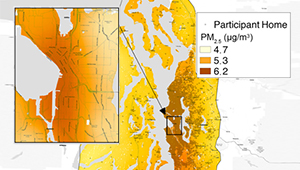
Air pollution linked to higher risk of dementia
With data from the ACT Study, researchers associated increased levels of fine particle pollution with a greater risk of dementia.
healthy findings blog

New Lancet report offers hope for preventing dementia
Dr. Eric B. Larson, a report contributor, answers questions about reducing risks, disparities, and threats from COVID-19.
Live Healthy

How to lower your risk of dementia
It’s never too late (or too soon) to take preventive steps.


