Electronic health records study offers insights on medical cannabis use
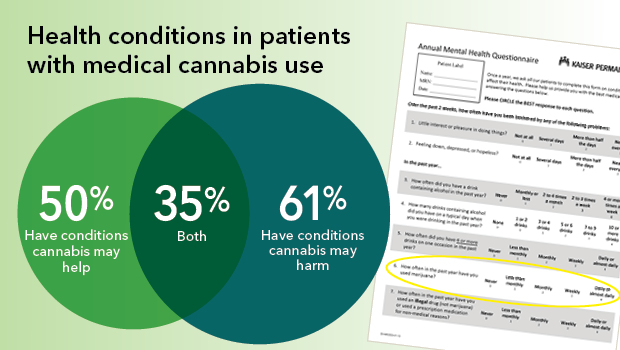
Data courtesy of Theresa Matson, Gwen Lapham, et al., Kaiser Permanente.
New research, led by KPWHRI investigators, examines providers’ notes to understand patients’ cannabis use and health conditions
Kaiser Permanente researchers have estimated, for what is believed to be the first time, the extent of cannabis use for medical reasons as documented in a health system’s electronic health records, or EHRs. The findings were published May 6 in JAMA Network Open.
The study found that patients with documentation of medical cannabis use are more likely to have health conditions that may benefit from cannabis use, as well as health conditions that may be worsened by cannabis use, than other patients. Furthermore, among patients with documented medical cannabis use, the prevalence of having both types of health conditions was significantly higher than among other patients.
“The study demonstrates that some patients are discussing medical cannabis use with their providers, and providers must be ready to have these complex conversations about the benefits and risks of cannabis with their patients,” said Theresa Matson, MPH, the study’s first author and a research interventionist at Kaiser Permanente Washington Health Research Institute. “If we consider these findings in the context of previous research suggesting providers feel unprepared to talk about medical cannabis, additional research and training on the health effects of cannabis use are needed.”
Matson and colleagues examined the EHRs of more than 180,000 primary care patients from November 2017 through October 2018 at Kaiser Permanente Washington, an integrated health system that conducts routine annual screening for cannabis use at primary care visits. Such routine screening for cannabis use is not yet implemented in most health care systems nationwide.
Along with using the screening data to identify patients who had reported cannabis use in the previous year, the researchers applied natural language processing to find documented cannabis use in providers’ EHR notes. Combined, about 2% of patients had documentation of medical cannabis use, and 20% had documentation of other (e.g., non-medical) use in their EHR. The remaining 78% had no indication of cannabis use in their records.
The researchers selected conditions that cannabis may either help or harm, as determined in a 2017 review from the National Academies of Science, Engineering, and Medicine, or NASEM. Among the conditions that NASEM identifies as potentially benefiting from cannabis are chronic non-cancer pain, multiple sclerosis, muscle spasms and spasticity, severe nausea, and sleep disorders. In turn, the report lists select mental health disorders, bronchitis, chronic obstructive pulmonary disease (COPD), substance use disorders, and opioid overdose as conditions associated with potential risk.
The study compares these health conditions’ prevalence among those with documented medical use of cannabis, those with documented other uses of cannabis, and those with no documented use of cannabis. It found:
- About half of the patients with medical cannabis use had health conditions for which cannabis has potential benefits. By comparison, 40% of patients with other or no cannabis use had such conditions.
- More than half (61%) of patients with documented medical cannabis use had health conditions that might be worsened by cannabis use. By comparison, 51% of patients with other cannabis use and 43% of patients with no use had such conditions.
- About 34% of patients with medical cannabis use had both types of conditions as compared with 25% of patients with other use and 22% of patients with no use.
Gwen Lapham, PhD, MPH, MSW, the study’s senior author and an assistant investigator at KPWHRI, said: “We know patients are using cannabis, and we now have a very good sense of what providers are documenting in the electronic health record around patients’ medical use of it. Our next step is to understand what patients report as their reasons for cannabis use and how much is captured in provider documentation. This will help us identify measures of cannabis use that reflect patient use, can be efficiently documented in patient EHRs, and ultimately inform patient-provider conversations about cannabis use.”
The study was made possible by funding from the National Institute of Drug Abuse Clinical Trials Network. In addition to Matson and Lapham, the study co-authors are David Carrell, PhD, Jennifer Bobb, PhD, David Cronkite, Malia Oliver, MS, Casey Luce, MSPH, Clarissa Hsu, PhD, and Katharine Bradley, MD, MPH, of KPWHRI; Udi Ghitza, PhD, of NIDA; Cynthia Campbell, PhD, MPH, of Kaiser Permanente Northern California Division of Research; Kendall Browne, PhD, and Andrew Saxon, MD, of Veteran Affairs Puget Sound Health Care System; and Ingrid A. Binswanger, MD, MPH, of Kaiser Permanente Colorado.
By Jonathan Rabinovitz
Open notes

Concerns about note-sharing fade with practice
A new federal rule requiring physicians to give patients access to their notes may be easier to follow than physicians expected.
innovating care

Asking patients about cannabis may benefit overall health
Drs. Lapham and Bradley find frequency of cannabis use can be tied to other behavioral health patterns and needs.
Healthy Findings Blog
Personal experiences inspire study of young adult patients and caregivers
Drs. Rosenberg and Wernli lead team with first-hand knowledge of complex conditions and care.
Read it in Healthy Findings.
Research

HEAL responds to double crisis: Opioids and COVID-19
Health care is increasingly online—KPWHRI is studying telehealth options for opioid use disorder and chronic pain.



