IUD perforation: Rare but important to know about
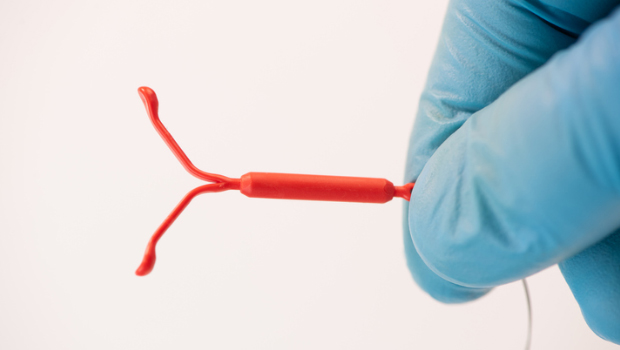
New study results in more precise language in the federally mandated warning about this possibility
Women who choose to use an intrauterine device, or IUD, for birth control should be aware of the very small possibility that the device could puncture their uterus. They should know how to recognize that circumstance if it occurs, according to a new study published in The Lancet.
The U.S. Food and Drug Administration mandated the study to evaluate women's risks when an IUD is placed in the year after giving birth and when an IUD is placed during the period that a woman is breastfeeding a baby. These results were compared, respectively, with non-postpartum insertions and insertions in non-breastfeeding individuals, explained Susan Reed, MD, MPH, MS, the study’s lead author. Dr. Reed is an affiliate investigator at Kaiser Permanente Washington Health Research Institute (KPWHRI) and an adjunct professor in epidemiology at the University of Washington School of Medicine.
Coauthors on the study include Laura Ichikawa, MS, a senior collaborative biostatistician at KPWHRI.
Across the study cohort, the percentage of perforation cases diagnosed within 5 years of IUD insertion was 0.6 %, the study concluded.
- The risk of perforation increased by nearly 7 times if the IUD was inserted between 4 days and 6 weeks postpartum, and the risk increased by about one-third if inserted during the span of breastfeeding.
- The risk of an IUD-related perforation was relatively lower when inserted in women who were more than a year beyond delivery, in women who had never had a baby, and when the insertion occurred at delivery.
Reed said the study led Bayer Pharmaceuticals to make a label update on its Mirena IUD, providing greater precision to the existing language. The packaging instructions alert women to contact their doctor immediately if they experience symptoms associated with uterine perforations. The main symptoms are pain and change in bleeding patterns, Reed said.
“This study provides additional information on which patients may be at higher risk of perforation and which patients may need additional monitoring. It is a reminder to providers that the consent process is critical and that we should provide better instructions on what to watch for,” said Reed, an ob-gyn with the University of Washington School of Medicine. As well, medical providers may ask patients who are experiencing symptoms to seek follow-up ultrasounds in clinic to ensure that the IUD is in the proper place.
Using health records, the study followed approximately 327,000 women age 50 or younger with IUD insertions from 2001 to 2018. Among the women, the researchers identified 1,008 uterine perforations involving IUDs that contained either copper or a progesterone hormone. The postpartum cohort (within 12 months of childbirth) comprised approximately one-third of the women in the study.
The data was collected from 3 health care systems — Kaiser Permanente Northern California, Kaiser Permanente Washington, and Kaiser Permanente Southern California — as well as a research site, the Regenstrief Institute, using data from a health care information exchange.
Despite the slight increase of perforation when insertion occurs in breastfeeding women and in women with insertions between 4 days and 6 weeks postpartum, “perforation remains an incredibly rare event," the report stated.
“The main takeaway is that follow-up may be warranted with these specific groups of patients,” Reed said. “We want to stress to women that this is a safe option for contraception.”
This has been adapted from a news story on this study by UW Medicine, University of Washington.
Research
New findings on treating hypertension in pregnancy
A study led by Dr. Sascha Dublin finds similar outcomes for 3 hypertension medications, filling an evidence gap.
ACT Study

Roundup of 3 recent studies on dementia risk
Researchers explore links between hearing loss, military service, and cognitive decline — and look at timeliness of diagnosis.
research

Medication in pregnancy: Better data for healthier kids
Researchers need much bigger data sets to find outcomes that matter, Dr. Sascha Dublin and colleagues write in Pediatrics.



