Roundup of 3 recent studies on breast cancer screening

New research spotlights overdiagnosis, MRI before surgery, and a new way of predicting breast cancer risk
Breast cancer screening is moving from "one size fits all" to recommendations that consider family history, age, and personal features such as breast density. Screening technology is also expanding — for example, with MRI (magnetic resonance imaging) and digital breast tomosynthesis. Three new studies based on data from the Breast Cancer Surveillance Consortium (BCSC), with leadership or contributions from researchers at Kaiser Permanente Washington Health Research Institute (KPWHRI), shed light on new screening recommendations and technology evaluations.
Revising overdiagnosis estimates
Overdiagnosis happens when screening detects cancers that would not have caused symptoms or otherwise been noticed or caused harm during the individual’s lifetime. How often it occurs is a topic of debate and sometimes confusion for researchers, clinicians, and individuals making personal decisions about breast screening. Overdiagnosis from screening leads to unneeded cancer treatment. Reliable estimates on the extent to which overdiagnosis occurs are crucial for creating screening guidelines.
A new paper on overdiagnosis with KPWHRI Senior Research Associate Ellen O’Meara, PhD, and affiliate investigator Diana Miglioretti, PhD, as coauthors was published in Annals of Internal Medicine. Using BCSC data for individuals ages 50 to 74, the researchers estimate that 15% of screen-detected breast cancers, about 1 in 7, are overdiagnosed in those who screen every other year. These results update previous estimates using simpler methods that suggested that, in general, overdiagnosis accounts for as many as 1 in 3 U.S. breast cancer diagnoses. The new study's methods consider what we know about the biology and progression of breast cancer to find that, among the overdiagnosed cancers in this group, one-third would not have progressed. The rest would not have led to clinical disease before death from other causes.
Writing for Fred Hutchinson Cancer Research Center, study senior author Ruth Etzioni, PhD, says, "While the results confirm that breast cancer overdiagnosis is real, they also reassure that it is not as alarmingly frequent as some studies have suggested." Co-author Ellen O'Meara, who co-leads the BCSC Biostatistical and Data Management Core with Diana Miglioretti, says the study is "just one example of the informative research supported by BCSC data, which reflect contemporary breast screening as it occurs in U.S. communities."
Evaluating preoperative MRI
As breast MRI becomes more common in community practices, determining when it offers meaningful benefits in screening and other situations is critical. This was the goal of a study in Breast Cancer Research and Treatment with KPWHRI coauthors Senior Collaborative Biostatistician WeiWei Zhu, MS, Associate Investigator Karen J. Wernli, PhD, previous Senior Investigator Diana Buist, PhD, and affiliate investigators Diana Miglioretti, PhD, Janie Lee, MD, MSc, and Christoph Lee, MD, MS.
Using BCSC data on breast cancer diagnoses from 2005 to 2017, the researchers evaluated the benefits and harms of MRI before surgery for newly diagnosed breast cancer. Preoperative MRI may be useful for determining the extent of disease and checking for additional cancer. Breast density, which contributes to breast cancer risk, was among the factors examined in the study.
The researchers found that for those in the sample with dense breasts, preoperative MRI was associated with much higher biopsy rates without the benefit of higher cancer detection. Study coauthor Karen Wernli says the results do not mean that use of MRI before breast cancer surgery is unhelpful. However, clinicians should be aware that the evidence does not support using breast density as a reason to recommend the procedure. Ongoing work from this team includes studying women's perceptions about using breast MRI in the diagnostic workup process and its impact on decision-making quality.
Predicting risk of advanced cancer
The fundamental goal of breast screening is detecting cancers in time to apply life-saving treatments. With that goal in mind, screening frequency may be every year, every other year, or some other interval. Individual decisions about screening frequency may be complex and depend on multiple personal factors. To help guide these decisions, BCSC researchers including previous KPWHRI Senior Investigator Diana Buist, PhD, and affiliate investigators Janie Lee, MD, MSc, and Diana Miglioretti, PhD, report in the Journal of the National Cancer Institute about a new method for predicting risk of advanced-stage breast cancer.
Using BCSC data for a sample group of people ages 40 to 74 who screened either every year or every other year, the researchers found risk differences that support screening annually for some and biannually for others. For most in the sampled group (69%), screening frequency did not affect their risk of being diagnosed with advanced breast cancer. For a group of 12% who had intermediate risk of advanced disease, however, more frequent screening lowered their risk to average. This group might consider annual instead of biannual screening. A remaining group had potentially higher risk that was unaffected by screening frequency. Individuals in this group might consider annual mammography screening supplemented with another method, such as MRI. The risk prediction model developed in the study is being developed into a BCSC online risk calculator.
co-researchers
Weiwei Zhu, MS
Principal Collaborative Biostatistician
Karen Wernli, PhD
Senior Investigator
researcher profile

What drives Karen Wernli to study breast cancer?
This Breast Cancer Awareness Month, Dr. Karen Wernli reflects on her cancer research, centered on patients and access.
Cancer screening
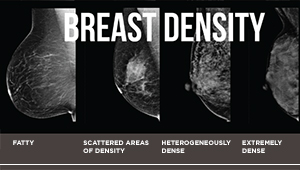
Breast density is a risk factor for older women, too
Findings in JAMA Network Open could help guide decision-making about breast cancer screening for women 75 and older.
Healthy findings blog

Prioritizing breast screening during COVID-19
As cancer screening rates rebound, Erin Bowles, MPH, reflects on maintaining “pink ribbon” awareness year-round.


