Cardiovascular Health
Research overview
Heart disease is the leading cause of death for Americans. Kaiser Permanente Washington Health Research Institute (KPWHRI) scientists are working to understand how to reduce our risk of heart attacks, stroke, and other cardiovascular diseases throughout life.
Addressing risk factors, improving diagnosis, and exploring how medications, genes, and everyday life affect our cardiovascular health at different ages and stages are central to this work — as is translating research findings into practical, personalized care.
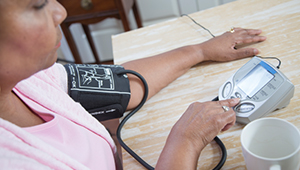
“We’ve found that helping patients and health care teams work together on personalized care plans is the best path to lifelong heart health,” says Beverly Green, MD, MPH, whose recent work has focused on improving the diagnosis of high blood pressure.
Additional focus areas for KPWHRI scientists include exploring the impact of cardiovascular diseases on other health conditions — and vice versa. Recently, this has led researchers Sascha Dublin, MD, PhD, and Laura B. Harrington, PhD, MPH, to investigate the impact of COVID-19 on cardiovascular health.
Below are other research highlights from KPWHRI’s cardiovascular health scientists (please visit their bios to learn more):
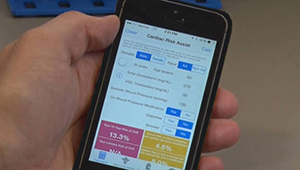
- In 2016 Dr. Green, a senior investigator, launched the BP-CHECK study, which aims to find the easiest, most accurate way to diagnose high blood pressure. With a $2.8 million award from the Patient-Centered Outcomes Research Institute (PCORI), the study compares blood pressure readings taken in clinic, at home, and at validated blood pressure kiosks to the 24-hour blood pressure test that is currently considered the gold standard for diagnosing hypertension.
- Dr. Dublin, a senior investigator, explores many different facets of cardiovascular disease in her work, including risk factors for atrial fibrillation, the effect of medications on cardiovascular disease, and the relationship between cardiovascular disease and other conditions, such as dementia. Managing cardiovascular risk factors in pregnancy — such as high blood pressure and diabetes — is a particular interest.
- Dr. Harrington, an assistant investigator, is a cardiovascular epidemiologist whose research aims to improve understanding of modifiable cardiovascular risk factors, particularly among older women. Currently, she is leading a study exploring the relationship between physical activity, sedentary behavior, and the risk of venous thromboembolism (blood clots that form predominantly in the veins of the legs or lungs). In addition to this work, Dr. Harrington conducts research in the areas of recurrent cardiovascular event risk, cardiovascular health in relation to cognitive decline and dementia risk in later life, and pharmacologic exposures in relation to cardiovascular event risk, with a particular focus on risk factors for venous thromboembolism.
- Senior Investigator Michael L. Parchman, MD, MPH, focuses on implementing evidence-based cardiovascular disease care into primary care settings. He led the 4-year Healthy Hearts Northwest trial, an EvidenceNOW initiative that helped smaller primary care practices in Washington, Oregon, and Idaho adopt evidence-based approaches to improving cardiovascular care outcomes. The trial continues to produce findings of importance.
- The work of Ellen O'Meara, PhD, a senior research associate, centers on the epidemiology of common and important health conditions in the United States, including cardiovascular disease. Her collaborative research has included studies exploring the risk factors and outcomes of heart disease and stroke. Recent work includes research on quality improvement aimed at controlling hypertension at small primary care practices.
Recent publications on Cardiovascular Health
LaCroix AZ, Haynes SG, Savage DD, Havlik RJ. Rose Questionnaire angina among United States black, white, and Mexican-American women and men. Prevalence and correlates from The Second National and Hispanic Health and Nutrition Examination Surveys. Am J Epidemiol. 1989;129(4):669-86. PubMed
Pieper C, LaCroix AZ, Karasek RA. The relation of psychosocial dimensions of work with coronary heart disease risk factors: a meta-analysis of five United States data bases. Am J Epidemiol. 1989;129(3):483-94. PubMed
Reed DM, LaCroix AZ, Karasek RA, Miller D, MacLean CA. Occupational strain and the incidence of coronary heart disease. Am J Epidemiol. 1989;129(3):495-502. PubMed
Ballard DJ, Strogatz DS, Wagner EH, Siscovick DS, James SA, Kleinbaum DG, Cutchin LM, Ibrahim MA. Hypertension control in a rural southern community: medical care process and dropping out. Am J Prev Med. 1988;4(3):133-9. PubMed
Newton KM, Killien MG. Patient and spouse learning needs during recovery from coronary artery bypass. Prog Cardiovasc Nurs. 1988;3(2):62-9. PubMed
Researchers in Cardiovascular Health
 Sascha Dublin, MD, PhDSenior Investigator |
 Beverly B. Green, MD, MPHSenior Investigator |
 Laura Harrington, PhD, MPHAssociate Investigator |
 Ellen O'Meara, PhDPrincipal Collaborative Scientist |
 Nicole M. Gatto, PhD, MPHPrincipal Collaborative Scientist |
 Meagan C. Brown, PhD, MPHAssistant Investigator |
Affiliate researchers
James Floyd, MD, MS
Assistant Professor, Department of Medicine
Adjunct Assistant Professor, Department of Epidemiology
University of Washington
Susan Heckbert, MD, PhD
University of Washington (UW) Department of Epidemiology; UW Cardiovascular Health Research Unit
Nicholas L. Smith, PhD, MPH
UW Professor, Epidemiology, Cardiovascular Health Research Unit
Director, Seattle Epidemiology and Information Resource Center, VA Puget Sound Health Care System