Making self-care videos in the age of pandemic

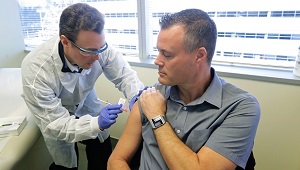
Clinical Nurse Specialist Meredith Cotton (bottom left) was featured in videos that Melissa Parson (top right) produced for patients learning to do their own insulin injections. (Photo credit for top left: Nirvana Van Horn-Ream)
Melissa Parson shares 4 lessons she learned while on assignment with Kaiser Permanente Washington diabetes nurses
By Melissa Parson, Kaiser Permanente Washington Health Research Institute video producer
It was the first week of the stay-at-home order in Seattle. I received a call from a number I didn’t recognize, but I’m glad I picked up. It was Jen Gee, a nurse who works with the population of Kaiser Permanente Washington patients who have diabetes. She was looking for someone to help her make two short videos instructing patients how to give themselves insulin injections, so they wouldn’t need to come into the clinic.
Jen called me because I am a video producer in Kaiser Permanente Washington Health Research Institute (KPWHRI). I typically create videos to share our research findings with the public. And while I had never worked with Kaiser Permanente nurses to create instructional videos, I had helped our researchers make videos for study participants on topics like mindfulness meditation, how to swab your own nose, and how to collect your own saliva samples. I have a reputation of sorts: You name it, Melissa will do it.
When I went to grad school for film, I never expected to be making videos on nasal swabs or insulin shots, but in truth, it feels right to contribute my skills in this way, especially now. My late grandfather Dr. William Parson, who encouraged me to get my MFA, was a beloved medical doctor and epidemiologist. He may not have cared for some of my more experimental videos, but I think he would have been so glad that I’m doing this work to help patients.
People with diabetes and other chronic illnesses are particularly vulnerable to COVID-19, so it’s critically important they know how to take care of themselves from the safety of their homes. The less they are exposed to others in places like doctor’s offices and emergency departments, the better. Video has become increasingly important for patients to learn new things during this pandemic.
I myself learned a few things as I prepared to make videos in the time of COVID. I have underlying medical conditions that put me at higher risk of complications if I were to get COVID-19. I was afraid to leave my house except for walks in the neighborhood. So even though Jen told me the video would be filmed in a clinic that was not currently seeing patients, my decision to take on the project was not a slam dunk. I debated with my husband, John, who is also my sound engineer, about whether we should make the videos. We had to think about how our exposure to others might affect our own well-being and that of our teenage son.
I called my trusted Aunt Polly, who is 79 years old, for advice. She and my uncle are in quarantine, leaving their house only once a week to drive their Prius, keeping the battery charged. They are smart, active, healthy, and staying safe, as they have lots of living still to do. I trust their opinions. If she said it was OK, I would feel better. And after family talks, both Polly and John thought we’d be fine—as long as we followed social-distancing guidelines and were extra cautious.
Here’s what the project taught me:
1. Be prepared!
Filmmaking is a fairly intimate process, normally done in quite close quarters. This became even more evident in the face of this pandemic. We needed to find masks, disposable gloves, and hand sanitizers, none of which were available in local or online stores at the beginning of the shut-down. But our online West Seattle “Buy Nothing” Facebook group came through for us. We would be able to have control in planning for this. I could call the shots—literally. Lights, camera, Purell!
I would also need to think about my equipment in new ways. For example, we normally would have had a free-standing “shot-gun” mic available, but we were restricted from the place where all of our equipment was stored; instead we had to use a lavaliere mic, which attaches to interviewees’ clothing. So John carefully cleaned the mic with alcohol wipes and instructed the wonderful nurse and spokesperson Meredith Cotton how to attach it herself.
2. 6 feet is 6 feet.
We also needed to think about what it means to be 6 feet away from our subject. I brought tape and marked the spots on the floor to keep social distancing in check. A few times, I felt myself slowly easing closer to Meredith to try to see the tiny numbers on the insulin pen. But then I would notice the visual markers, which helped to keep us all safe.
3. Don’t let perfection be the enemy of the good.
My office was closed so I couldn’t gather all my equipment, but I made do with what I had on hand. John and I have seen the late-night comedy hosts like Colbert, Fallon, and Kimmel filming at home. Even on their shows, it’s clear that during a pandemic, content is more important than production values. As long I could clearly see and hear the subject, it would be OK. And normally, I’d have insisted on having the script early enough to create a complete “shot list,” but this piece was written by a dedicated nurse the day before shooting. So we flew by the seat of our pants, trusting that it was better to just get the work done because the patients needed it right away.
4. Make sure it feels right.
The fear I felt didn’t totally go away. But we moved forward, knowing there were people counting on us. John had said he thought the project was a noble thing to do, and he said there would likely be more needs like this in the future.
Although I agreed, I still couldn’t sleep the night before we filmed. But when the daylight came, it felt right. I knew we were “all in.”
We used our fear to keep us mindful of the necessary precautions.
We thought about the patients who need the information and need it now. And, of course, we thought about all the courageous nurses who make the choice to keep working through the pandemic. They walk the talk to improve care for their patients every day, and to help keep them at home and safe.
John and I are proud to be part of this important effort.
Melissa Parson wishes to thank the KPWHRI Innovation Fund for its support of the diabetes self-care video project, which is now posted online for patient use. Jen Gee and Meredith Cotton say the videos provide the clear and simple guidance patients need to do their own insulin injections at home.
Healthy Findings Blog
How epidemiologists predict the future of COVID-19
KPWHRI’s Dr. Michael Jackson describes how better testing will improve our ability to forecast the pandemic’s path.
director's note
Research versus COVID-19
From clinical trials to technical support, Dr. Rita Mangione-Smith describes how Kaiser Permanente Washington researchers are fighting the novel coronavirus.
news

Diabetes is more common among minorities at lower weights
At normal weight, Pacific Islanders are 3 times likelier than whites to have diabetes, Kaiser Permanente research finds.


