Treating hypertension in pregnancy: What’s the best way?
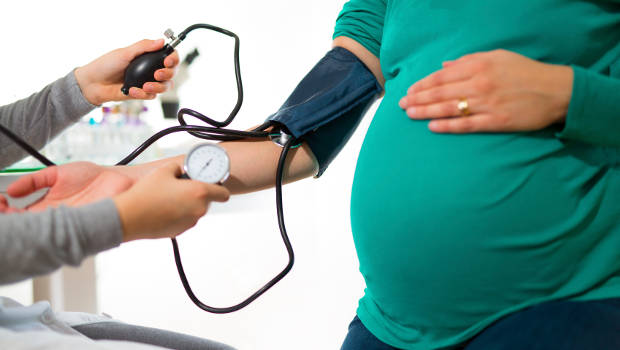
A GHRI study by Dr. Sascha Dublin uses data from pregnant women’s experiences to find out the risks and benefits of taking high blood pressure medicine.
Hypertension (high blood pressure) affects approximately 300,000 pregnant women in the United States each year, but doctors have little clinical evidence to guide treatment decisions—including whether to prescribe medications and if so, which ones. Group Health Research Institute associate investigator and Group Health physician Sascha Dublin, MD, PhD, is working to change that. With colleagues from the University of Washington and Kaiser Permanente, she is leading one of the largest studies ever of the impact of hypertension medications on maternal and fetal health, including looking at differences by race/ethnicity and obesity status.
When a pregnant woman has high blood pressure, the risks to her health and that of the fetus increase significantly. Hypertensive disorders are one of the leading causes of maternal deaths worldwide. But both doctors and mothers can be hesitant about medications because they don’t know if treatment could result in harm to the unborn baby.
Hypertension and pregnancy
Even women with no history of high blood pressure can develop hypertension in pregnancy because of changes that occur in the body, including a rise in the amount of blood that begins in the first trimester. The heart has to work harder to move the increased blood. High blood pressure results in increased health risks for the mother, and in some cases can decrease the flow of blood to the placenta, causing reduced birth weight or fetal death in the uterus.
One advantage of taking hypertension medication, in addition to direct benefit to the mother, could be a higher likelihood of carrying the pregnancy to full term. But many women are reluctant to take medication out of fear of harming their baby.
“There are three parts to the puzzle,” Dr. Dublin explains. “How do you keep the mom healthy? How do you keep the baby healthy? And how do you help the pregnancy continue until as close to the due date as possible?”
Lack of evidence
A major review article combined data from many randomized trials and reported that only 4,200 women worldwide had participated in trials of medication use for mild-to-moderate hypertension in pregnancy. Of these, only about 1,280 women were in studies comparing outcomes from different drugs. According to Dr. Dublin, “In the past, a typical randomized trial included about 100 women.” As a result, doctors and mothers have limited evidence for assessing risks and making appropriate decisions.
In contrast, Dr. Dublin estimates that her study will include information from about 30,000 pregnancies in electronic health record (EHR) data from Group Health, Kaiser Permanente Southern California, and Kaiser Permanente Northern California, as well as state birth and fetal death records. The EHR allows researchers to use real-world clinical data from pregnancies complicated by mild-to-moderate hypertension to determine how maternal and infant outcomes differ in treated and untreated women and if outcomes differ by medication type, race/ethnicity, and obesity status of the women.
Research and mothers’ well-being
We are becoming more aware of the impact of a pregnant or lactating woman’s choices on the health of her baby. Not only are smoking and drinking actively discouraged, there is heightened concern about the impact of any medication during pregnancy.
The question of the safety and effectiveness of hypertension medication is related to a larger problem: the lack of information about most medications’ impact during pregnancy.
Dr. Dublin raises the concern that in many cases, women with serious health conditions may be scared to take a medication with an unclear safety profile—even though sometimes, avoiding medications may do more harm than good.
“I think in our society in general, we spend a lot of time thinking about whether or not pregnant women are taking too many drugs,” says Dr. Dublin. “We might not spend as much time thinking about drugs women need for conditions like depression, lupus, or inflammatory bowel disease, but don’t take because they are afraid to do so during pregnancy.”
Not taking medications can also cause problems. "These women experience suffering because of their symptoms. If their medical problem is not under good control, this could also have a negative impact on their babies,” Dr. Dublin says.
“My concern is it could be that many women are needlessly deprived of medicines that might help them and their baby do better, if we had the data to understand their actual impact.” —Dr. Sascha Dublin
According to some prior studies, 95 percent of women in the U.S. take some kind of medication during pregnancy. In many cases, the data about their outcomes are there to be studied in EHR and other records. With all this information available, why don’t we know more? Randomized trials are usually considered the “gold standard” for studying medications, but these studies are very expensive. Also, randomly assigning women to take medicines with unknown safety in pregnancy may be unethical.
Use of EHR data to study medication safety in pregnancy is certainly increasing, but these studies can be criticized because some information is missing, for instance, women’s use of over-the-counter medications, or exposure to tobacco or alcohol. These factors could affect pregnancy outcomes and potentially cause study bias.
“We have come a long way in developing sophisticated methods for using these data,” says Dr. Dublin. “So hopefully, we are entering a new era in which we can greatly increase the amount of information available to women and doctors.”
Dr. Dublin’s study represents a huge step forward in understanding how to better care for women and their unborn babies. The results from this study could have an immediate impact on clinical practice, helping women and providers make more informed choices together, which could result in healthier women and healthier babies.
by Janet Hendrickson, MS
Dr. Dublin’s project is funded by a grant of more than $3.8 million from the Eunice Kennedy Shriver National Institute of Child Health and Human Development.
healthy findings blog

Tough conversations: How can we help patients get off risky drugs?
Dr. Sascha Dublin describes a Group Health-UW finding that benzodiazepines probably don’t cause dementia. But she cautions that they’re still bad for you.
Read it in Healthy Findings.
Group Health Research News September 2016
In this issue
- Treating hypertension in pregnancy: What’s the best way?
- Bariatric surgery keeps weight off in long term
- Biostatistician Yates Coley returns to Seattle as new investigator
- Preventing dementia: A long-term ACT idea goes mainstream
- Sustaining diabetes self-management programs: Community members speak
- The world seems unstable but are there some constants in health?
- Carol Cahill of GHRI bicycles to honor husband and fund cancer research
- The Weeds has health IT questions, we have answers


