Eric A. Johnson, MS
Biography
Eric Johnson, MS, completed the University of Washington’s biostatistics master’s program in 2008. His thesis explored common theoretical problems involved with missing data. He quantified them, highlighting conditions leading to suboptimal performance, and provided new guidelines for using various multiple imputation techniques.
During his time at KPWHRI, Mr. Johnson has been involved with multiple projects involving direct intervention with the care-delivery system, observational studies and microsimulation modeling on colorectal and ovarian cancer, massage therapy, and estimating radiation exposure from medical imaging. His current responsibilities lie in research on obesity, opioids, and mental health.
Before earning his master’s degree, Mr. Johnson worked for four years as a research assistant on the Multi-Ethnic Study of Atherosclerosis (MESA), performing statistical analyses, verifying incoming data, and developing a process for providing data sets to all MESA researchers. Later, he was a research statistician with the Department of Veteran Affairs (VA), serving as the primary analyst in an investigation of how well VA hospitals performed non-cardiac surgeries. Mr. Johnson assessed statistical models used by the National Surgical Quality Improvement Program—then devised, tested, and implemented improved models, reporting his findings to VA leadership.
Research interests and experience
-
Biostatistics
Multiple imputation; prediction models, working with large data
-
Health Systems
Implementing prediction models, and validating that they work as intended. Research into interventions that are financially feasible for health systems to widely implement
-
Cancer
-
Complementary & Integrative Health
-
Health Services & Economics
-
Obesity
-
Mental Health
Recent publications
Coley RY, Johnson E, Simon GE, Cruz M, Shortreed SM. Racial/ethnic disparities in the performance of prediction models for death by suicide after mental health visits. JAMA Psychiatry. 2021 Apr 28:e210493. doi: 10.1001/jamapsychiatry.2021.0493. [Epub ahead of print]. PubMed
Coleman KJ, Shu YH, Fischer H, Johnson E, Yoon TK, Taylor B, Imam T, DeRose S, Haneuse S, Herrinton LJ, Fisher D, Li RA, Theis MK, Liu L, Courcoulas AP, Smith DH, Arterburn DE, Friedman AN. Bariatric surgery and risk of death in persons with chronic kidney disease. Ann Surg. 2021 Mar 3. doi: 10.1097/SLA.000000000000485. [Epub ahead of print]. PubMed
Tsui JI, Akosile MA, Lapham GT, Boudreau DM, Johnson EA, Bobb JF, Binswanger IA, Yarborough BJH, Glass JE, Rossom RC, Murphy MT, Cunningham CO, Arnsten JH, Thakral M, Saxon AJ, Merrill JO, Samet JH, Bart GB, Campbell CI, Loree AM, Silva A, Stotts AL, Ahmedani B, Braciszewski JM, Hechter RC, Northrup TF, Horigian VE, Bradley KA. Prevalence and medication treatment of opioid use disorder among primary care patients with hepatitis C and HIV. J Gen Intern Med. 2021 Feb 10. doi: 10.1007/s11606-020-06389-7. [Epub ahead of print]. PubMed
Koffman L, Levis AW, Arterburn D, Coleman KJ, Herrinton LJ, Cooper J, Ewing J, Fischer H, Fraser JR, Johnson E, Taylor B, Theis MK, Liu L, Courcoulas A, Li R, Fisher DP, Amsden L, Haneuse S. Investigating bias from missing data in an electronic health records-based study of weight loss after bariatric surgery. Obes Surg. 2021 Jan 19. doi: 10.1007/s11695-021-05226-y. [Epub ahead of print]. PubMed
Matson TE, Lapham GT, Bobb JF, Johnson E, Richards JE, Lee AK, Bradley KA, Glass JE. Cannabis use, other drug use, and risk of subsequent acute care in primary care patients. Drug Alcohol Depend. 2020 Aug 8;216:108227. doi: 10.1016/j.drugalcdep.2020.108227. [Epub ahead of print]. PubMed
Arterburn DE, Johnson E, Coleman KJ, Herrinton LJ, Courcoulas AP, Fisher D, Li RA, Theis MK, Liu L, Fraser JR, Haneuse S. Weight outcomes of sleeve gastrectomy and gastric bypass compared to nonsurgical treatment. Ann Surg. 2020 Mar 13. doi: 10.1097/SLA.0000000000003826. [Epub ahead of print]. PubMed
Boudreau DM, Lapham G, Johnson EA, Bobb JF, Matthews AG, McCormack J, Liu D, Samet JH, Campbell CI, Rossom RC, Binswanger IA, Yarborough BJH, Arnsten JH, Cunningham CO, Glass JE, Murphy MT, Zare M, Hechter R, Ahmedani B, Braciszewski JM, Horigian VE, Szapocznik J, Samet JH, Saxon AJ, Schwartz RP, Bradley KA. Documented opioid use disorder and its treatment in primary care patients across six US health systems. J Subst Abuse Treat. 2020 Mar;112S:41-48. doi: 10.1016/j.jsat.2020.02.001. PubMed
Lapham G, Boudreau DM, Johnson EA, Bobb JF, Matthews AG, McCormack J, Liu D, Samet JH, Saxon AJ, Campbell CI, Glass JE, Rossom RC, Murphy MT, Binswanger IA, Yarborough BJH, Bradley KA. Prevalence and treatment of opioid use disorders among primary care patients in six health systems. Drug Alcohol Depend. 2020;207:107732. doi: 10.1016/j.drugalcdep.2019.107732. Epub 2019 Nov 15. PubMed
Carrell DS, Albertson-Junkans L, Ramaprasan A, Scull G, Mackwood M, Johnson E, Cronkite DJ, Baer A, Hansen K, Green CA, Hazlehurst BL, Janoff SL, Coplan PM, DeVeaugh-Geiss A, Grijalva CG, Liang C, Enger CL, Lange J, Shortreed SM, Von Korff M. Measuring problem prescription opioid use among patients receiving long-term opioid analgesic treatment: development and evaluation of an algorithm for use in EHR and claims data. J Drug Assess. 2020 Apr 28;9(1):97-105. doi: 10.1080/21556660.2020.1750419. eCollection 2020. PubMed
Simon GE, Shortreed SM, Johnson E, Rossom RC, Lynch FL, Ziebell R, Penfold ARB. What health records data are required for accurate prediction of suicidal behavior? J Am Med Inform Assoc. 2019 Dec 1;26(12):1458-1465. doi: 10.1093/jamia/ocz136. PubMed
Research

Study finds bariatric surgery linked to substantially lower risk of blood clots long-term
Largest study to date helps patients weigh risks and benefits of surgery.
New findings

Simpler models to identify suicide risk perform similarly to more complex ones
Models that are easier to explain, use could have better uptake in health care settings.
New findings

Research roundup on natural language processing and machine learning
Using doctor's notes to learn about drug reactions, dementia, and cannabis use.
New findings
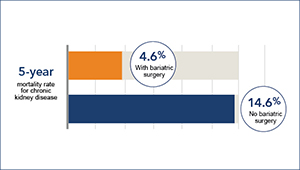
Is bariatric surgery helpful in chronic kidney disease?
David Arterburn and colleagues find that bariatric surgery is linked to lower death risk in persons with obesity and CKD.



